Cadaver Experiences
Studies by sociologists have found that no experience has a more profound impact on medical school students than the first encounter with death, which typically occurs during the first-year course of gross anatomy. With its required dissection of human cadavers, the course seeks to impart a variety of explicit lessons, including the size, shape, and exact location of organs varies from one individual to another; organs vary in their "feel" and texture and are connected to other parts of the body in complex ways that textbook illustrations cannot effectively reproduce; and surgical instruments have specific purposes and must be handled properly to avoid injury to the patient or oneself. A less explicit, but no less important, result is overcoming the natural emotional repugnance at handling a cadaver.
First-year medical students report having the most difficulty dissecting those parts of the body with strong emotional associations, especially the hands, face, and genitals, as opposed to the arms, legs, and abdomen, which can more easily be bracketed as mere physical body parts. One common method of dealing with the emotional upset of cadaver dissection is the use of humor—students often circulate cadaver stories as a test of one another's proper emotional preparation through humor involving a dismembered corpse.
Cadaver stories. Cadaver stories (jokes involving anatomy-lab cadavers) have been studied by researchers interested in urban folklore. Researchers have found that most of these stories are unlikely to be true and that they fall into five basic categories, all connected with the emotional socialization of medical students:
- Stories describing the removal of cadaver parts outside of the lab to shock ordinary citizens (mailing body parts to friends or handing change to a toll collector with a severed hand are examples of this category).
- Manipulation of the cadaver's sexual organs which shocks or offends another medical student.
- The cadaver appearing to come to life at an unexpected time, supposedly frightening a novice student. One such story features a medical student taking the place of the cadaver under the sheet; at the right moment, the student twitches and then sits upright to the screams of the emotionally unprepared.
- Stories featuring the cadaver as a food receptacle. Students may claim to have heard of a student in another lab who hid food in a corpse and later removed and ate it during class. Like the previous type of story, this category is supposed to test the queasiness of medical students who are expected to find the story amusing.
- The realization that the medical student has finished dissecting a member of his or her own family (the head is the last part of the cadaver to be dissected and because it is so emotionally charged, it is almost always kept covered until the end of the anatomy course).
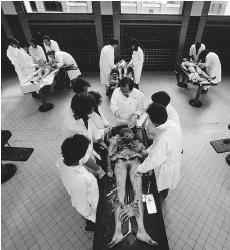
Stories of this last kind have more credibility with medical students than those in the first four categories, which require conscious misbehavior on the part of some other medical student. In this cadaver story, a well-prepared medical student is still capable of being emotionally assaulted by the realization that she has spent the entire semester dissecting her own mother. Although such an event is highly unlikely, some physicians are obliged to operate on a friend or someone resembling a family member.
Taken together, cadaver stories reveal the common need for medical students to verbalize their discomfort with death and dead bodies. While the stories are about medical students or emotionally squeamish laypersons, the students reciting these legends are themselves skittish and use the stories as a type of emotional fortification.
Dog labs. A second stage in the emotional socialization of medical students is associated with socalled dog labs that, until recently, were found in many medical schools. In dog labs, medical students operate on anesthetized dogs supplied by local animal-control shelters. Unlike cadavers, these creatures are alive and must be kept alive during dissection. Overt learning outcomes include familiarity with anesthetics, care in working on a living creature that bleeds and needs to be kept breathing, and additional training in the use of surgical instruments. A less explicit outcome is another lesson in emotional socialization because the dogs are expected to die on the operating table. Anesthetized and thus incapable of feeling pain, the animals are given a fatal drug overdose. Recently, this practice has been eliminated from most medical schools, but for years it was considered a necessary step in preparing the student to work on living human patients.
Witnessing an autopsy. The third component in preparing future physicians for dealing with death involves attending and participating in an actual autopsy. Usually scheduled for the second year of medical school training, the autopsy moves students closer to what had very recently been a living human being. Unaffected by preservatives, the body's organs look and feel exactly as they would on the operating table, allowing students an opportunity to collect information even closer to the real thing. At this point, most students report that they have arrived at a new stage in emotional detachment from death. Shorn of the protective layer of cadaver stories, students use the scientific knowledge gained during their many chemistry and biology classes as a bulwark against emotional distress. Students report that cadaver dissection does not completely prepare them for the autopsy, and some experience difficulty remaining in the room during the procedure.
Patients with terminal illnesses. Having reached their third and fourth years of medical school, students begin to come into contact with actual patients. Some of these patients are terminally ill and represent a new challenge to emotional control and response to the prospect of death. None of the previous stages prepare students for interaction with a patient whose death is imminent. By this point in their education, some students report that they are troubled by their desensitization to the suffering and deaths of patients and fear that they will come to resemble the icy, hardened practitioners they have always despised. By the fourth year of medical school, however, most students report an overcoming of this feared detachment and an attainment of a proper emotional balance.
Changes in Medical School
This sequence of stages in emotional socialization coincides with stages in the training of medical students. For many years, that training was fairly uniform among medical schools. Similarly, the sorts of students enrolling in medical school often shared certain characteristics: male, white, twenty-two to twenty-five years of age, middle- to upper-middle-class background, a thorough grounding in the hard sciences, and a high grade point average from a reputable undergraduate institution. By the end of the twentieth century, however, significant changes occurred in the training of medical students, who were increasingly likely to be female, non-white, and to have taken many non-science courses. These developments may mean that the model of emotional socialization for confronting death is changing. For example, many medical schools now routinely bring medical students into contact with patients during their first year. Although this usually involves taking medical histories or simply overcoming discomfort in speaking with strangers about their health problems, it may well affect the manner in which emotional detachment develops. Also, cadaver stories appear to be evolving. Initially, many stories featured female medical students as their target. Analysts interpreted this as a thinly veiled form of sexism. Recently, however, stories have appeared that feature pranks backfiring against male perpetrators. In another shift in gross anatomy labs, female students sometimes choose to work together in dissection of female cadavers, believing that male students do not show proper respect for female genitalia.
The studies summarized above describe the experience at institutions offering training in conventional allopathic medicine. Nontraditional medical training (e.g., homeopathy or chiropractic) may produce a very different set of reactions in the encounter with death. Likewise, the confrontation with death in medical schools in other countries varies with the unique cultural mores that have shaped the students.
See also: Autopsy ; Death Education ; Nursing Education
Bibliography
Fox, Renee C. The Sociology of Medicine: A Participant Observer's View. Englewood Cliffs, NJ: Prentice Hall, 1989.
Furst, Lilian R. Between Doctors and Patients: The Changing Balance of Power. Charlottesville: University of Virginia Press, 1998.
Hafferty, Frederic W. "Cadaver Stories and the Emotional Socialization of Medical Students." Journal of Health and Social Behavior 29, no. 4 (1988):344–356.
Lantos, John. Do We Still Need Doctors? A Physician's Personal Account of Practicing Medicine Today. New York: Routledge, 1997.
Lawton, Julia. The Dying Process: Patients' Experiences of Palliative Care. London: Routledge, 2000.
Magee, Mike, and Michael D'Antonio. The Best Medicine: Doctors, Patients, and the Covenant of Caring. New York: St. Martin's Press, 1999.
Tauber, Alfred I. Confessions of a Medicine Man: An Essay in Popular Philosophy. Cambridge: MIT Press, 1999.
JONATHAN F. LEWIS
Comment about this article, ask questions, or add new information about this topic: